Histamine is well-known for playing a role in the allergic response, even if most people only recognize the word histamine due to a connection with antihistamines as allergy medication. But lately, it has also become identified as a potential source for food intolerance. Does it deserve to be maligned as a potentially harmful component of food? Let’s see what the literature has to say.
What Is Histamine?
Histamine does much more than play a role in the allergic response. Let’s take a brief look at histamine and its role in the body before diving into dietary histamine and whether it is harmful.
Several cells synthesize and use histamine, including mast cells, basophils, platelets, histaminergic neurons, and enterochromaffin cells (cells in the stomach tissue that play a role in the production of gastric acid). It is one of the molecules stored in vesicles and then released when needed.
As one of its many functions in the body, histamine is a neurotransmitter with roles in mediating arousal, reactivity, anxiety, sleep-wake cycle, and attention. Histamine does not cross the blood-brain barrier; instead, the amino acid histidine (its precursor) enters the brain to synthesize into histamine through a reaction requiring histidine decarboxylase.
There are four receptors for histamine, known as H1R, H2R, H3R, and H4R. These receptors are found in various tissues throughout the body and may be involved in one or more of the following:
- Blood pressure alterations
- Circadian rhythm
- Gastric acid secretion
- Immunomodulation
- Vascular permeability
- Intestinal ischemia
- Mucus secretion
- Neurotransmission
- Smooth muscle contraction
- Tachycardia and/or arrhythmias
- Vasodilation
- Wound healing

Some studies show that in addition to playing a role in acute inflammation response (e.g., allergic response), it may also be a part of chronic inflammation, which may play a role in diseases associated with chronic inflammation atherosclerosis. Histamine may also regulate glucose and lipid metabolism and thus protect against non-alcoholic fatty liver disease.
It also plays a role in appetite control, and stimulation of histamine H1 receptors can inhibit leptin and act as an anorexigenic (appetite-lowering) agent. It may play a role in obesity treatment.
Histamine plays several key roles in the body, but it also needs to be broken down and metabolized, or it will overwhelm the body and cause problems. Two enzymes do this: DAO (diamine oxidase) and HNMT (histamine N-methyltransferase). DAO is most associated with histamine breakdown and histamine intolerance (and the one most studied in connection with dietary histamine and histamine intolerance and thus the one discussed in more detail in this blog). HNMT only acts intercellularly while DAO acts in circulation and can scavenge for extracellular histamine. DAO is mostly found in the intestines, placenta, and kidney.
The body synthesizes the histamine it requires, but it is also found in many foods. Foods that contain higher levels of histamine include:
- Avocado
- Cheese
- Eggplant
- Fermented foods
- Fish, especially dried fish
- Salami and other hard-cured sausages
- Spinach
- Tomato
- Wine

Different cooking methods may also impact histamine levels, with one study showing that frying and grilling led to an increase in histamine while boiling had a neutral or lowering effect.
Histamine Intolerance
Dietary histamine can increase serum levels of histamine. Normally, DAO works to prevent the uptake of dietary histamine. Still, in cases of low DAO or excessive histamine (as well as certain gastrointestinal disorders and dysbiosis in the gut microbiome), dietary histamine can trigger symptoms due to excess histamine, a condition known as histamine intolerance.
Histamine intolerance arises when the intake of histamine is more than the body’s ability to degrade it. It is different from histamine intoxication, a type of food poisoning, which occurs when there are abnormally large amounts of histamine in the food and is more common in fish and certain ripened cheese.
Common symptoms associated with histamine intolerance include:
- Abdominal pain
- Bloating
- Constipation
- Diarrhea and vomiting
- Flushing
- Headaches and migraines
- Increased heart rate (tachycardia)
- Itching
- Rhinitis
- Skin rash
- Urticaria (hives)
According to one study, histamine intolerance also commonly occurs along with other intolerances, namely fructose and lactose malabsorption, in those with unexplained GI symptoms. In this study, 26.4% of the participants had an overlap of lactose malabsorption, fructose malabsorption, and/or histamine intolerance, with a combination of lactose malabsorption and histamine intolerance more common. In those who had carbohydrate malabsorption, 36.9% also had histamine intolerance.
Genetics
Genetic polymorphisms are linked to reduced DAO activity, but not everyone with one of the SNPs will exhibit histamine intolerance signs. Although some people exhibit histamine intolerance due to genetic causes, many have secondary histamine intolerance due to medications and GI problems. Although histamine intolerance is getting a lot more press, estimates state that roughly one percent of the population has it.
Diagnostic Criteria
The diagnostic criteria for histamine intolerance usually consist of low-serum DAO and GI symptoms that improve upon a low-histamine diet. However, it is not a perfect way to find everyone affected by histamine in their diet. In one study, only 24% of suspected histamine-intolerant patients had high-histamine levels and low-DAO activity. The other patients had similar symptoms but did not have alternations in their histamine or DAO levels.
In another study, there was a correlation between low-DAO levels and migraine, with 87% of the group with migraines also falling into a category of DAO deficiency, compared to 44% in those without migraines. Low-DAO levels have also been associated with high-risk pregnancies and complications during pregnancy. One study also found that a subgroup of patients with eczema also had low-DAO activity.
Addressing Histamine Intolerance
As histamine intolerance becomes more established as a potential cause of food-allergy-type symptoms, researchers and physicians look for ways to address it. At this point, there are two options undergoing review: low-histamine diet and DAO supplementation, with some studies adopting both methods. Both methods have been found effective in at least some of the participants.
In one study, a low-histamine diet for at least three weeks significantly improved chronic spontaneous urticaria symptoms (i.e., hives) in about 75% of the study participants. However, another study did not show a link between histamine intolerance and hives despite almost half of the patients in the study improving on a low-histamine diet.
Another study also found a significant benefit of consuming a histamine-free diet for four weeks in chronic urticaria. Another small study found symptoms worsening in 30% of the patients with atopic dermatitis when they consumed a high-histamine diet.
Studies have also started looking at the benefit of supplementing with DAO for those deficient. In one randomized controlled trial on patients with migraines who met the criteria for DAO deficiency, those taking the supplement experienced a significant reduction in the hours of pain they experienced, with a mean of 6.14 hours before the treatment and 4.76 hours after the intervention. The placebo group also experienced a reduction in pain hours, but it did not reach statistical significance.
Another study found that supplementing with DAO for 30 days reduced the severity of chronic hives. There was an inverse relationship between improvement in the UAS-7 score (a measurement of disease severity) and serum DAO levels. In another small study in those with histamine intolerance, DAO supplementation reduced at least one symptom in 13 out of 14 patients.
Plant Compounds
There are plant and nutritional compounds with an antihistamine reputation due to their benefits in allergenic diseases, such as quercetin, nettle, resveratrol, and vitamin C. But would these also help with histamine intolerance and/or dietary histamine?
Thus far, the evidence is slim looking at these plant compounds on dietary histamine, DAO insufficiency, and/or histamine intolerance rather than in connection with the release of histamine from mast cells and other components of histamine’s role in the immune system. For example, studies point to quercetin’s benefits relating to its ability to inhibit histamine release from mast cells. However, quercetin does have additional benefits on the immune system and health beyond its antihistamine qualities, including anti-inflammatory, immunomodulatory, and antioxidant properties. Resveratrol has also been shown to inhibit histamine release and decrease the number of immune cells (dendritic cells, B cells, and mast cells), benefiting allergenic diseases, including food allergies. A mechanistic study found that nettle also inhibits mast cell degranulation and acts as an antagonist for the H1 receptor. A combination supplement to help with histamine is Hista-Eze.
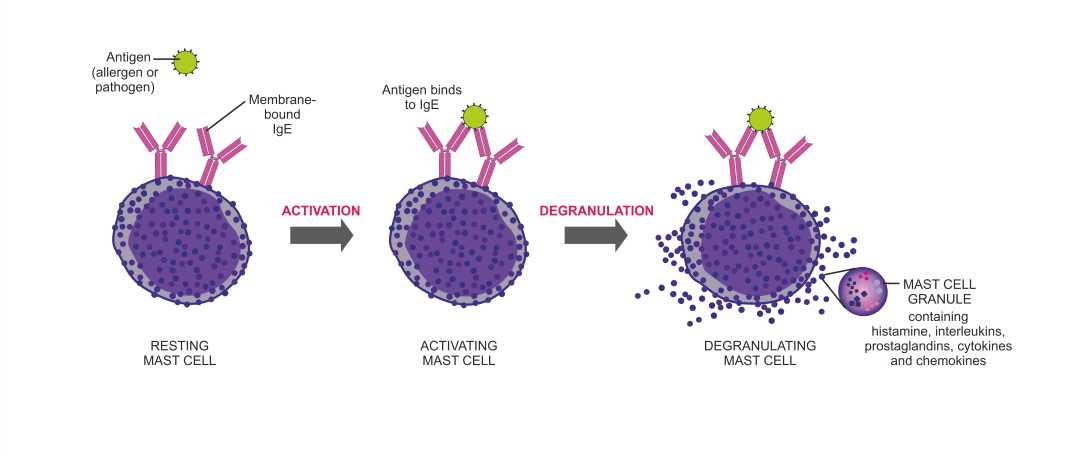
Photo: Soleil Nordic/Shutterstock.com
Vitamin C acts differently on histamine, making it more beneficial in histamine intolerance because it stimulates DAO activity. One study found that IV vitamin C reduced serum histamine levels, which was greater in those with allergenic diseases than infectious diseases. Additional studies have found an inverse association between vitamin C deficiency and histamine levels in the blood. Liposomal Vitamin C gets into the cells, similar to IV vitamin C.
Some of these elements may benefit those with an adverse reaction to histamine in food, but more research is necessary to determine what supplement or complementary foods work best. Additionally, in cases where there may be an underlying cause, such as those with GI disorders or dysbiosis, treating the root cause may also benefit and allow a person to resume consuming high-histamine foods.
Although histamine intolerance may be discussed more and more, the literature does not support its common condition. However, in those who have GI problems and/or food allergies who are not finding answers or relief, histamine intolerance may be worth investigating to see whether it is behind the symptoms. If you suspect you may be sensitive to histamine in foods, talk to your doctor, nutritionist, and/or another healthcare practitioner to determine the best course of action for you.

